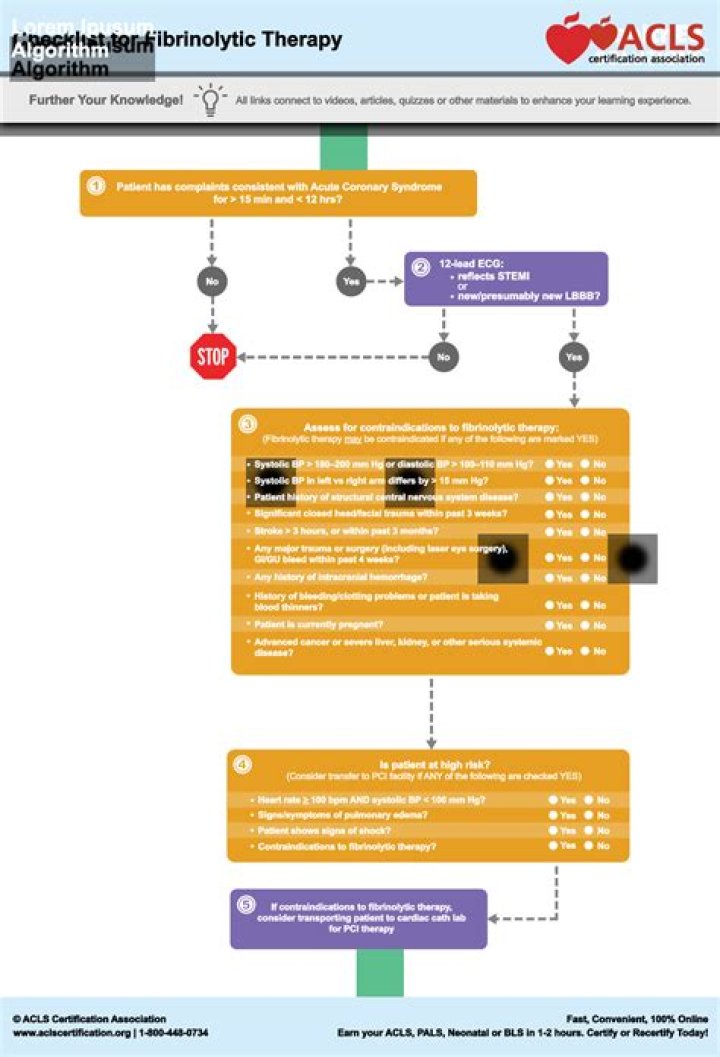
Who is not a candidate for fibrinolytic therapy?
Patients who have uncontrolled hypertension with a systolic blood pressure of greater than 180 mm Hg or a diastolic of greater than 110 mm Hg may also be excluded. Blood glucose levels are also taken into consideration. A glucose concentration of less than 50 mg/dL is considered a contraindication.
When can you not give fibrinolytic therapy?
Relative contraindications (not absolute) to fibrinolytic therapy include: Uncontrolled hypertension (BP > 180/110), either currently or in the past. Intracranial abnormality not listed as absolute contraindication (i.e. benign intracranial tumor) Ischemic stroke more than 3 months prior.
What are absolute contraindications to fibrinolytic therapy in a CV event?
Absolute contraindications Presence of a cerebral vascular malformation or a primary or metastatic intracranial malignancy. Symptoms or signs suggestive of an aortic dissection. A bleeding diathesis or active bleeding, (menstruation is an exception)
For which reason would a patient be excluded from receiving rtPA within 3 to 4.5 hours from the onset of a stroke?
Uncontrolled hypertension to values exceeding a systolic of 185 mm Hg or diastolic of 110 mm Hg is an exclusion criterion to IV rtPA according to the 2013 AHA guidelines and the drug label. This is likely derived from an exclusion criterion for the National Institute of Neurological Disorders and Stroke (NINDS) trials.
When is a fibrinolytic checklist required?
Fibrinolytic Checklist: Must be completed prior to administration.
What is the time goal for initiation of fibrinolytic therapy in appropriate patients without contraindication after hospital arrival?
Begin fibrinolytic therapy within 60 minutes of patient arrival to the ED. Consider endovascular therapy for the onset of symptoms up to 24 hours and large vessel occlusion. Admit the patient to stroke care within 3 hours of arrival to the ED.
What is the time goal for initiation of fibrinolytic therapy in appropriate patients without contraindications after hospital arrival?
What is fibrinolytic therapy and what are the major concerns and contraindications?
The contraindications for fibrinolytic therapy include previous intracranial hemorrhage, malignant intracranial neoplasm, known structural cerebrovascular lesion (e.g., arteriovenous malformation), ischemic stroke within 3 months except for acute ischemic stroke within 4.5 h, significant facial trauma or closed-head …
What is the diastolic threshold for withholding fibrinolytic therapy to otherwise eligible patients with acute ischemic stroke?
At the same time, guidelines recommend a conservative approach, with careful blood pressure lowering to a systolic pressure of 185 and a diastolic pressure of 110 mmHg before the start of thrombolytic treatment1 and maintenance of a pressure <180/110 mmHg, but we also know little about the effects of blood pressure– …
Which of the following criteria must be met in order to consider a patient eligible for treatment with Activase?
With a platelet count <100,000/mm, international normalized ratio (INR) >1.7, activated partial thromboplastin time (aPTT) >40 seconds, or prothrombin time (PT) >15 seconds.
Why is there no tPA after 3 hours?
“From analyzing all the available data, tPA [tissue plasminogen activator] after 3 hours for stroke patients may not be of any benefit but has a definite risk of fatal bleeding,” Dr Alper told Medscape Medical News.
When is fibrinolytic therapy indicated?
Fibrinolytic therapy may also be indicated if the signs and symptoms of a myocardial infarction last longer than 15 minutes and less than 12 hours and if PCI (percutaneous coronary intervention) is not available within 90 minutes of medical contact.