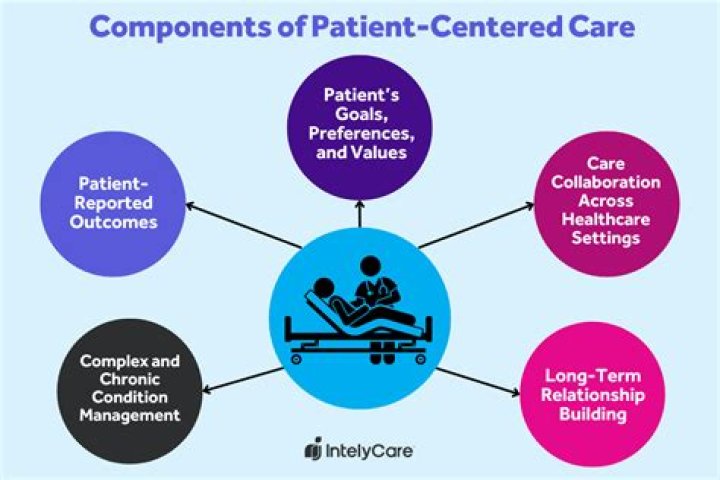
What is patient-centered care in healthcare?
Patient-centered care focuses on the patient and the individual’s particular health care needs. Patient-centered care is associated with a higher rate of patient satisfaction, adherence to suggested lifestyle changes and prescribed treatment, better outcomes and more cost-effective care.
What is an example of patient centered care?
Providing accommodations for family and friends. Involving family and close friends in decision making. Supporting family members as caregivers. Recognizing the needs of family and friends.
What is the primary goal of patient centered care?
The primary goal and benefit of patient-centered care is to improve individual health outcomes, not just population health outcomes, although population outcomes may also improve.
What is an example of patient-centered care?
Why is patient-centered care important?
According to a systematic review conducted by Rathert and colleagues [11], organizations that are more patient-centered also have more positive outcomes, such as greater satisfaction with care, greater job satisfaction among healthcare professionals, increased quality and safety of care, and greater quality of life and …
What is the importance of patient centered care?
Patient-centered care (PCC) has the potential to make care more tailored to the needs of patients with multi-morbidity. PCC can be defined as “providing care that is respectful of and responsive to individual patient preferences, needs, and values and ensuring that patient values guide all clinical decisions” [9].
How do you accomplish patient centered care?
Make sure the patient’s family and caretakers are fully vested in your care plan and understand the patient’s physical limitations, dietary requirements, and medication schedules. Help them coordinate ongoing treatments and ensure they’re informed about access to physical, financial, clinical, and social support.
What are the benefits of person centered care?
Benefits of patient-centered care
- Improved outcomes.
- Improved patient satisfaction.
- Improved reputation for your organization.
- Better job satisfaction for staff.
- Make healthcare accessible.
- Respect patients’ values, needs, and preferences.
- Coordinate care.
- Inform and educate your patients.
What are the benefits of coordination of care?
Greater coordination of care—across providers and across settings—will improve quality care, improve outcomes, and reduce spending, especially attributed to unnecessary hospitalization, unnecessary emergency department utilization, repeated diagnostic testing, repeated medical histories, multiple prescriptions, and adverse drug interactions.
What are the key factors driving healthcare transformation?
Factors driving healthcare transformation include fragmentation, access problems, unsustainable costs, suboptimal outcomes, and disparities. Cost and quality concerns along with changing social and disease-type demographics created the greatest urgency for the need for change.
What are the transformative changes happening in healthcare?
There are transformative changes occurring in healthcare for which nurses, because of their role, their education, and the respect they have earned, are well positioned to contribute to and lead.