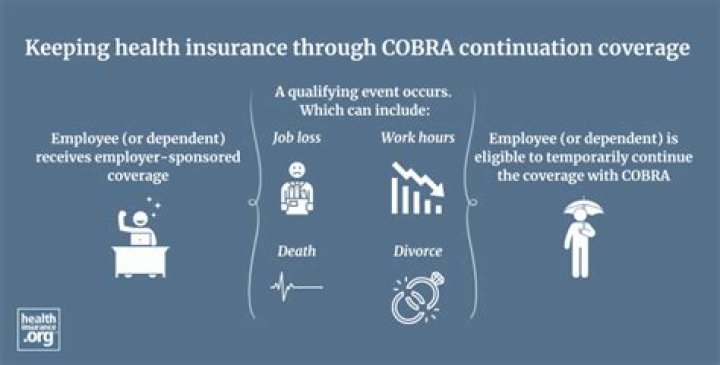
What is Cobra in health care insurance?
The Consolidated Omnibus Budget Reconciliation Act (COBRA) gives workers and their families who lose their health benefits the right to choose to continue group health benefits provided by their group health plan for limited periods of time under certain circumstances such as voluntary or involuntary job loss.
How much is Cobra health insurance per month?
On Average, The Monthly COBRA Premium Cost Is $400 – 700 Per Person. Continuing on an employer’s major medical health plan with COBRA is expensive. You are now responsible for the entire insurance premium, whereas your previous employer subsidized a portion of that as a work benefit.
Who qualifies for Cobra coverage?
COBRA covers group health plans sponsored by an employer (private-sector or state/local government) that employed at least 20 employees on more than 50 percent of its typical business days in the previous calendar year. Both full- and part- time employees are counted to determine whether a plan is subject to COBRA.
Is Cobra insurance a good deal?
That’s because health insurance is required for almost all Americans. One option is to buy a plan from the health insurance marketplace that was set up under the Affordable Care Act….Who’s eligible for COBRA health insurance.
| COBRA health insurance eligibility | |
|---|---|
| Your child turns 26, losing dependent status. | 36 months |
How does COBRA insurance work if I quit my job?
Named for the Consolidated Omnibus Budget Reconciliation Act of 1985, COBRA allows you to continue receiving the exact same health coverage you’ve been getting from your employer after leaving the company, as long as you weren’t fired for gross misconduct and you’re not covered by another plan elsewhere.
Does COBRA coverage begin immediately?
You have 60 days to choose a plan, and your benefits will start the first day of the month after you lose your insurance.
Is everyone eligible for COBRA?
Not everyone is entitled to elect COBRA continuation coverage. In general, COBRA benefits are only available for those covered by a group health plan maintained by an employer with 20 or more employees. Your employer can confirm your eligibility for COBRA or Cal-COBRA continuation coverage.
Does COBRA cost the employer?
Who pays for COBRA coverage? The employee generally pays the full cost of the insurance premiums. In fact, the law allows the employer to charge 102 percent of the premium, and to keep the 2 percent to cover your administrative costs.
Is COBRA cheaper than individual insurance?
Is COBRA cheaper than individual insurance? COBRA health insurance is usually more expensive than individual insurance, especially if you qualify for ACA plan subsidies. ACA subsidies reduce the cost of ACA plans. The subsidies are only eligible for ACA plans.