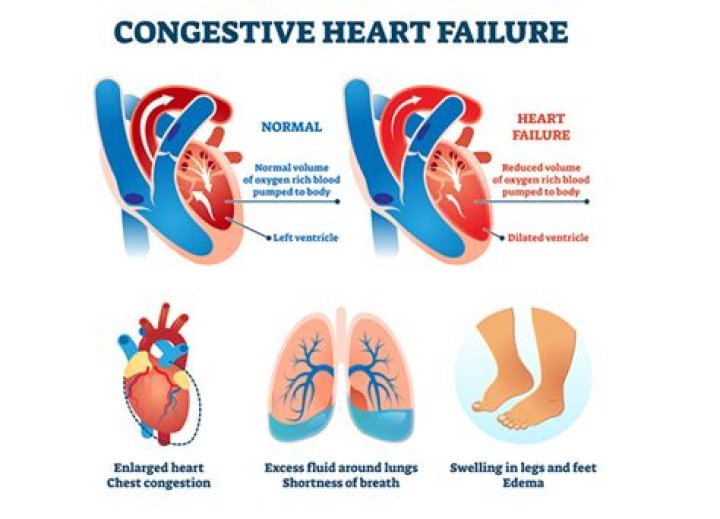
Can MI cause congestive heart failure?
Heart failure (HF) is a common complication of myocardial infarction (MI), which may develop early or late and persist, resolve or recur. A growing proportion of patients with MI are aged > 65 years. Older patients are at greater risk of developing HF and have a poorer prognosis.
Why does heart failure occur after MI?
Heart failure developing after MI hospitalization is a consequence of cardiomyocyte death and scar formation, which triggers chronic neurohumoral activation (renin–angiotensin–aldosterone and sympathetic nervous system up-regulation) and ventricular remodelling.
Why is heart failure a complication of MI?
Heart failure complicates 25-50 per cent of acute MIs arising from the loss of contractility in the damaged myocardium as left ventricular remodelling occurs. It tends to develop insidiously during the first few days following MI.
What are the main causes of myocardial infarction?
A heart attack occurs when one of the heart’s coronary arteries is blocked suddenly or has extremely slow blood flow. A heart attack also is called a myocardial infarction. The usual cause of sudden blockage in a coronary artery is the formation of a blood clot (thrombus).
What are the complications of acute MI?
With the above anatomical correlates in mind, the various complications of acute MI are easier to explain:
- Arrhythmias / Heart block:
- Hypotension:
- Ventricular septal rupture:
- Left ventricular free wall rupture:
- Left ventricular aneurysm formation:
- Right ventricular infarction:
What is the most common complication of MI?
VFWR is the most serious complication of AMI. VFWR is usually associated with large transmural infarctions and antecedent infarct expansion. It is the most common cause of death, second only to LV failure, and it accounts for 15-30% of the deaths associated with AMI.